Feeding hospitalized cats
Written by Rene Dorfelt
When should a cat be fed? Basically, as soon as possible. If anorexia is or may be present for more than 3 days. In kittens after a few hours of anorexia. As soon as cardiovascular and hemodynamic parameters are stable; major electrolyte abnormalities such as hyperkalemia should be corrected before feeding commences.
When should a cat be fed?
• Basically, as soon as possible!• If anorexia is or may be present for more than 3 days
• In kittens after a few hours of anorexia
• As soon as cardiovascular and hemodynamic parameters are stable; major electrolyte abnormalities such as hyperkalemia should be corrected before feeding commences
• Within 24 hours of presentation
• Within 6-12 hours following gastrointestinal surgery
What diet should be offered?
• Tasty food with a pleasant odor
• Consider starting with some “treats” to stimulate appetite
• A critical care diet with high energy and high protein content
• Food should be at room temperature
How should the cat be fed?
• Enteral if possible
• Partial parenteral if enteral nutrition does not provide adequate energy intake
• Parenteral nutrition if enteral nutrition is not possible
What is the best way to stimulate appetite?
• Use highly palatable food
• Create a cat-friendly, calm environment with soft, warm bedding and a place to hide
• Make sure the cat is not in pain; administer analgesia as appropriate
• Give anti-emetics and gastric protectants if the cat appears nauseous
• Appetite in cats is stimulated by smell; clean the cat’s nose if obstructed with mucus or other material
• Offer fresh food at room temperature on a regular basis
What about appetite-stimulating drugs?
• May be used if conventional techniques do not work
• Cyproheptadine is an H1-antihistaminic drug (1-4 mg/cat every 12-24h PO)
• Mirtazapine is a 5-HT3 antagonist (3-4 mg/cat every 3 days PO)
• Benzodiazepines (e.g., midazolam) may be used as a short-term option if other drugs fail. They may induce appetite at a very low dose (0.05 mg/kg IV) but may also cause sedation. However, hepatic failure has been described after giving diazepam to cats
What if the cat will not eat?
• Careful force-feeding using a syringe may be carried out if other techniques fail. It may also be beneficial to put some food on the cat’s paws, as the cat may lick it off whilst trying to clean itself
• Feeding tubes should be used if enteral feeding is possible, but the energy requirements are not fulfilled by spontaneous food intake
Naso-esophageal feeding tube
• Easy to place without general anesthesia
• Can be removed whenever required
• Usable for three or more days
• Only suitable for liquid diets
Materials required:
• Feeding tube 4.5-6 FG
• Lidocaine-containing lubricant
• Suture material
• Needle holder
• Scissors
Placement technique:
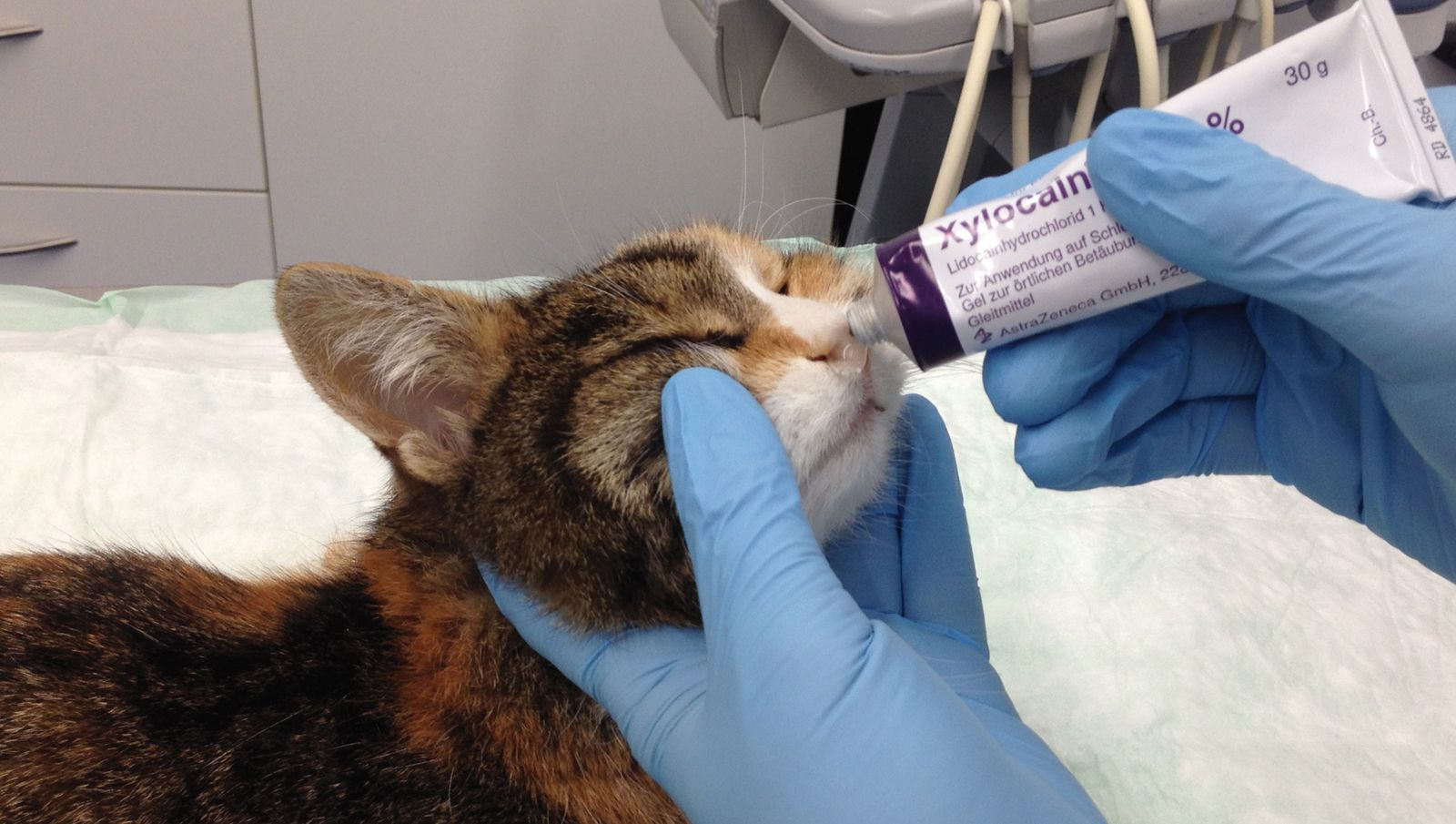
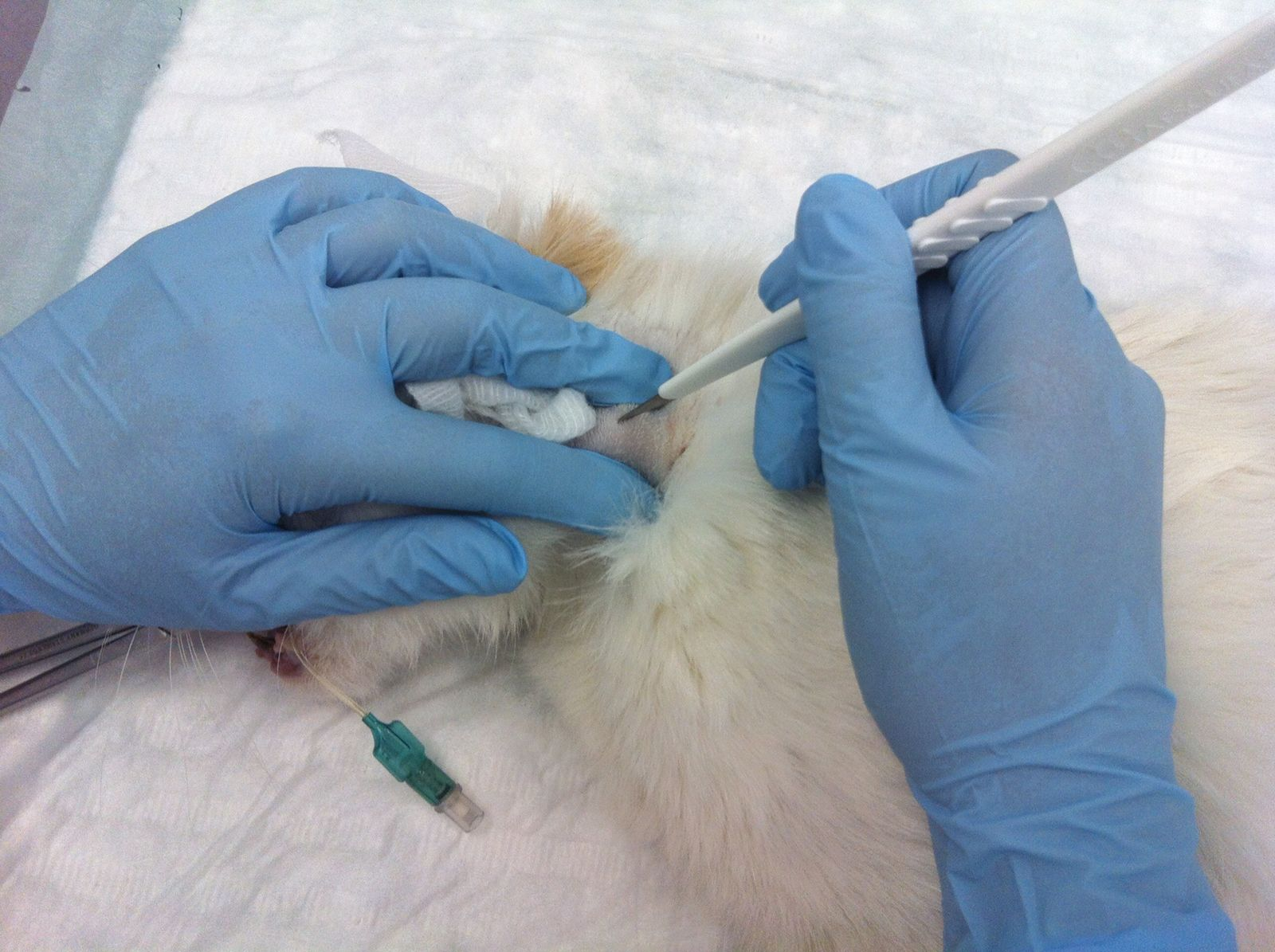
• Place some lubricant on the lower nasal meatus and at the tip of the tube (Figure 1)
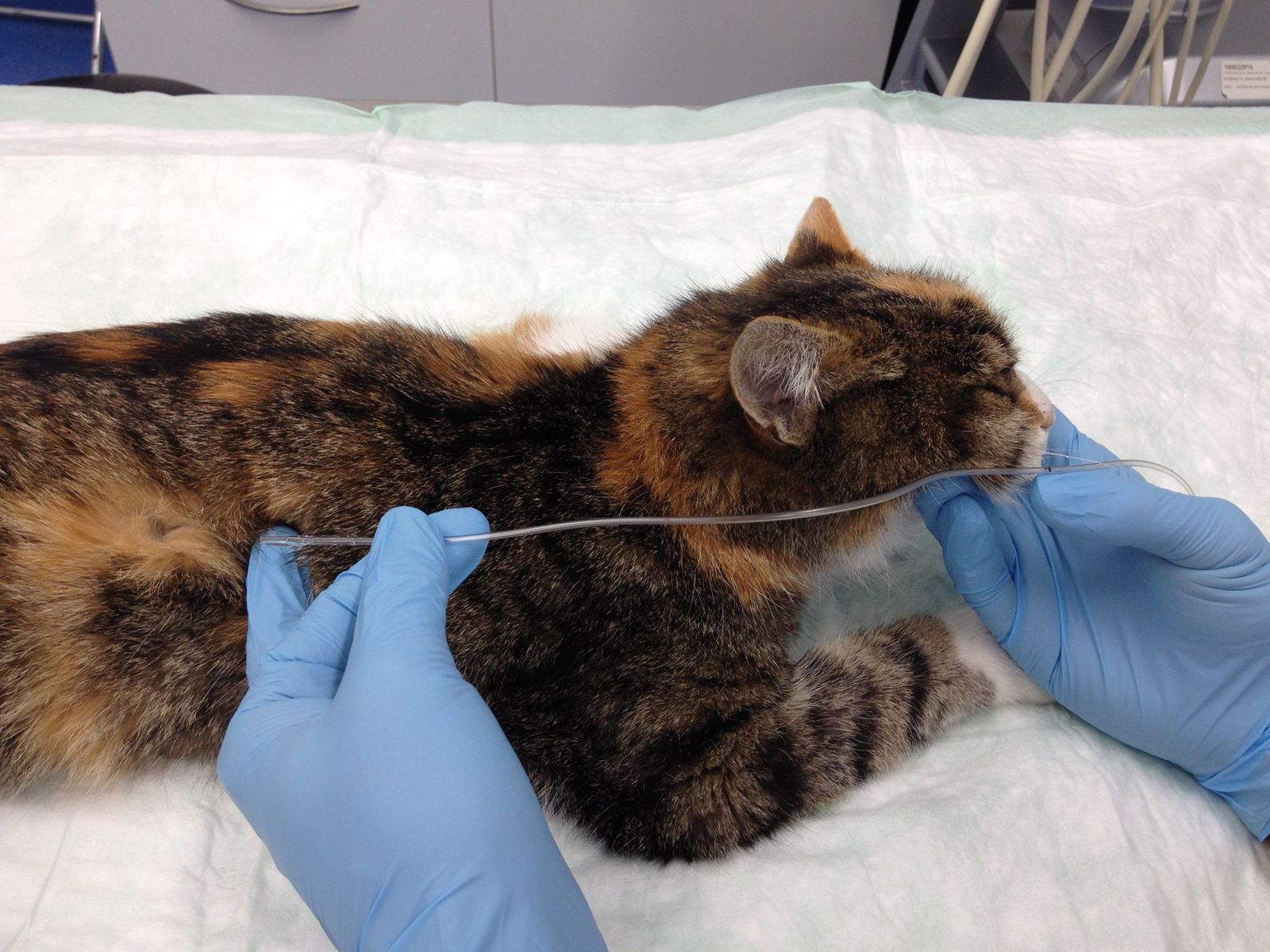
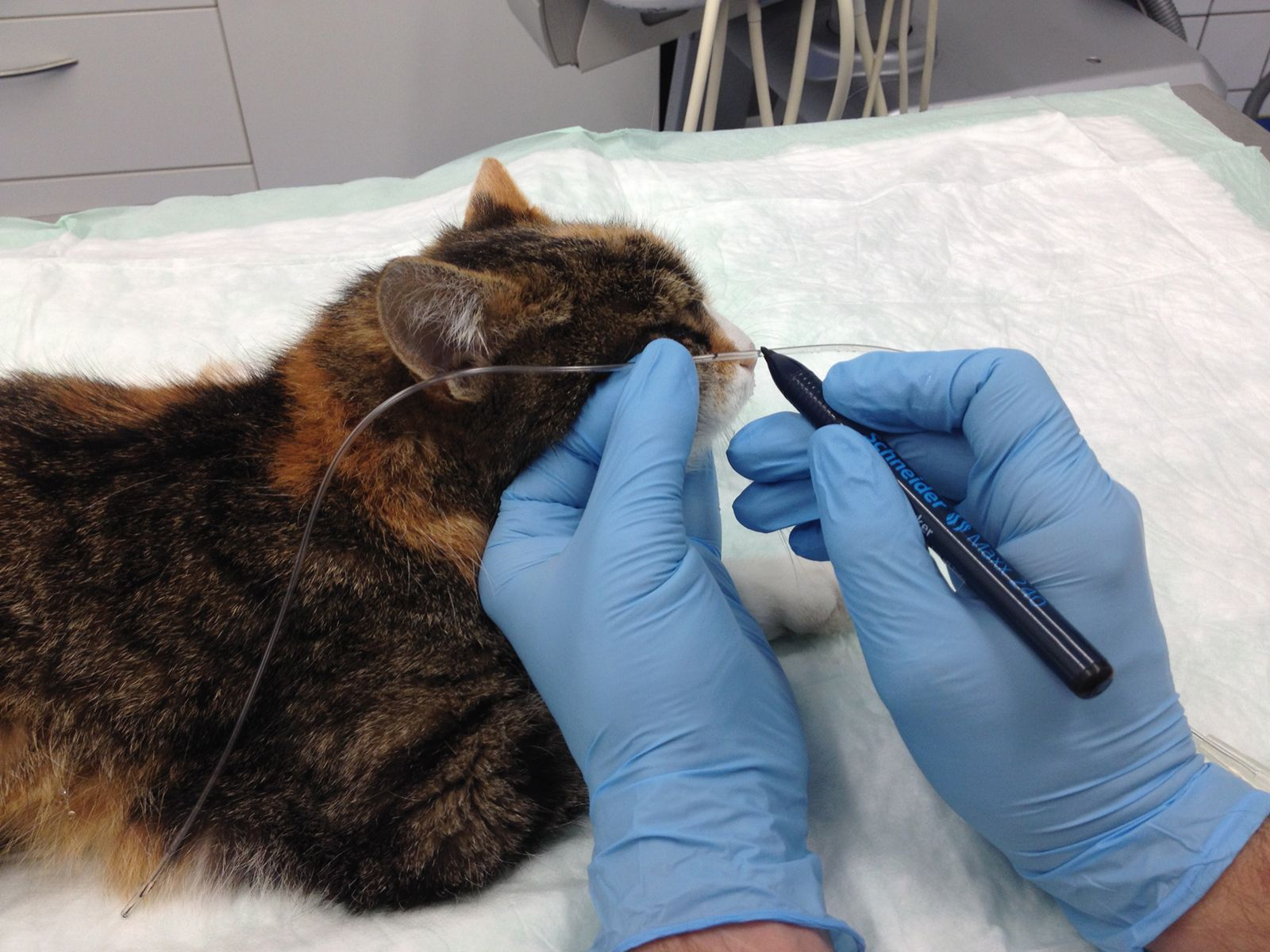
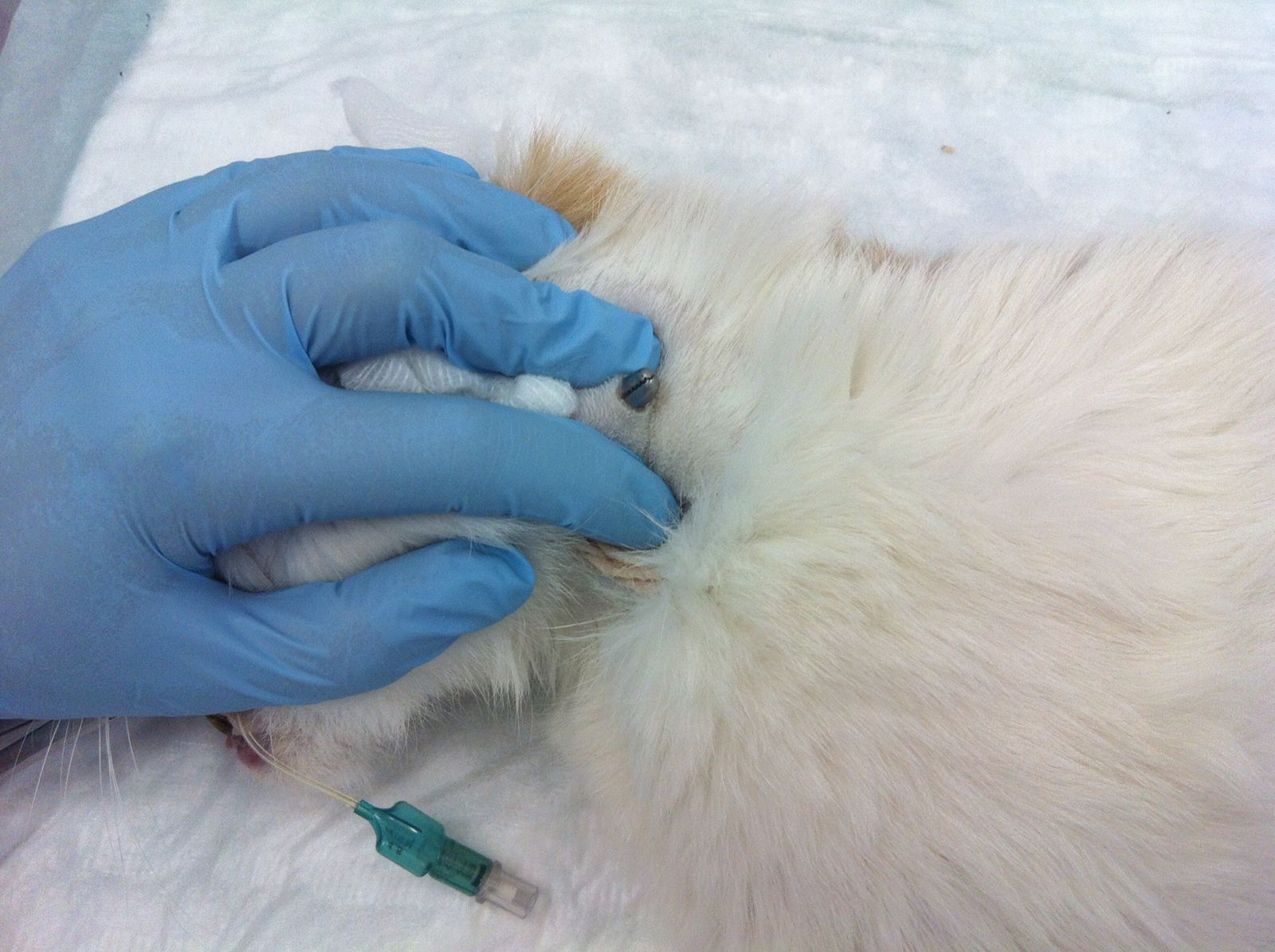
• Measure tube length from the nose to the 8th intercostal space and mark with a permanent marker (Figure 2 and 3)
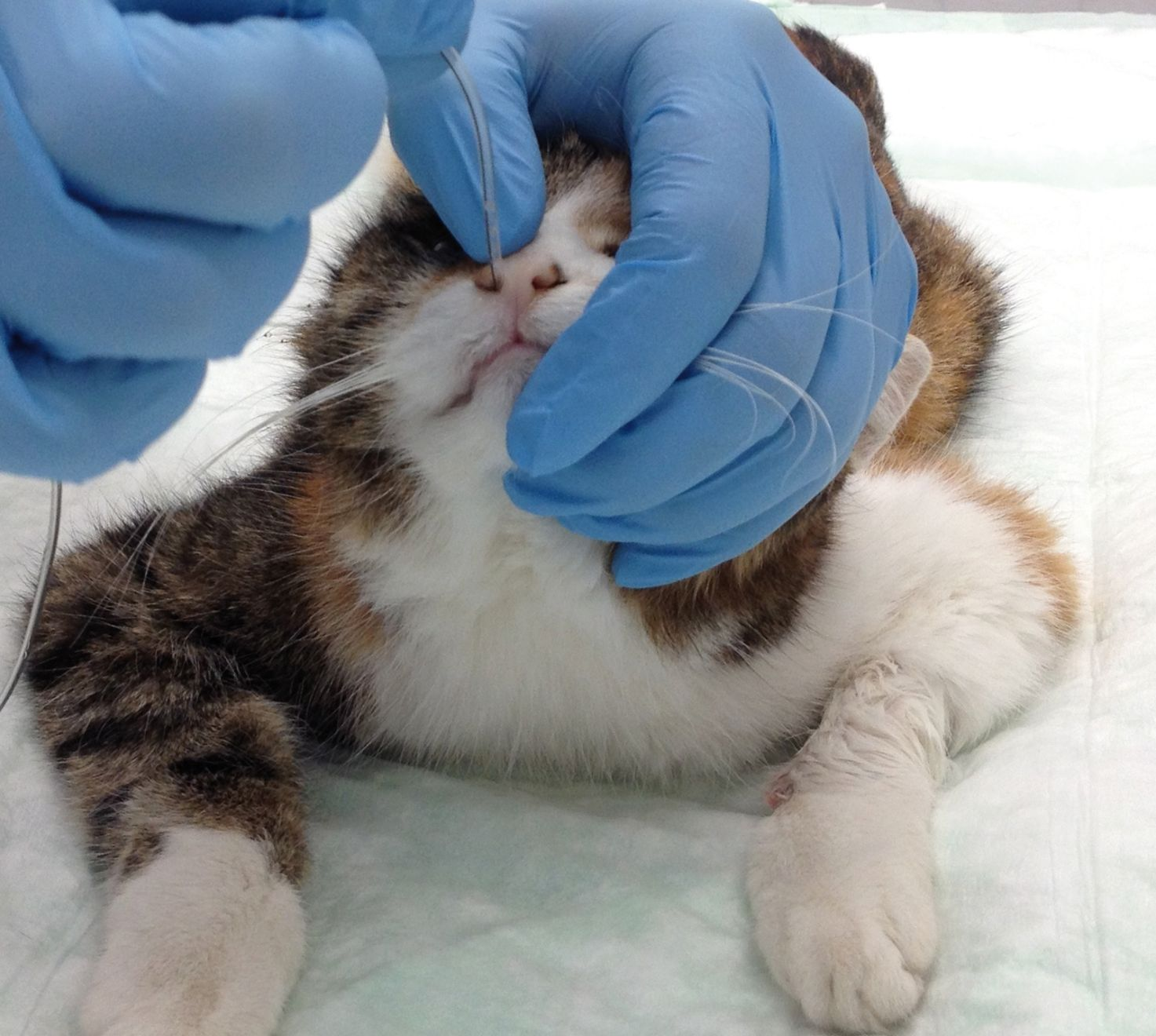
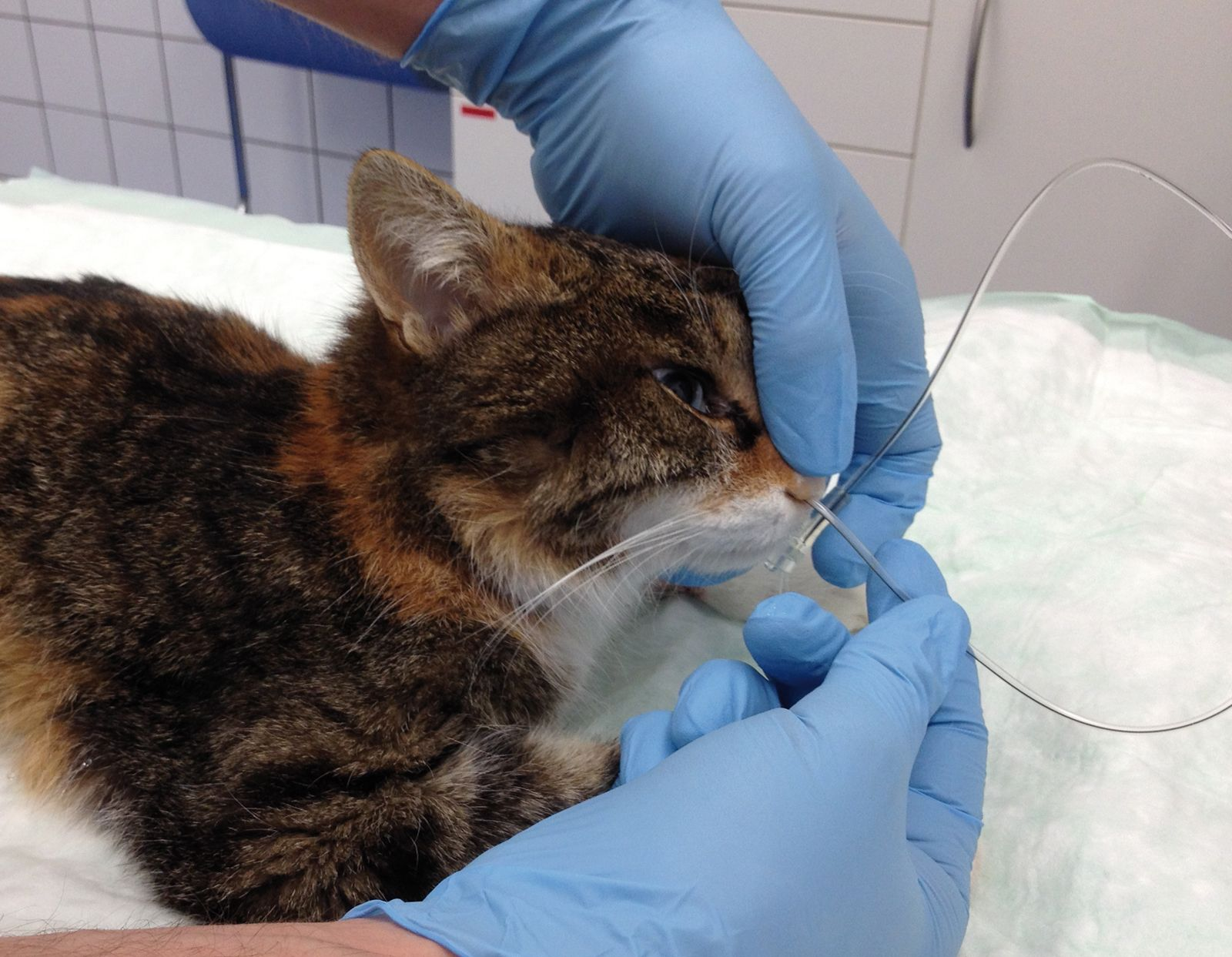
• Introduce the tube into the lower nasal meatus by directing the tube tip ventro-medially (Figure 4)
• Allow the cat to swallow the tube by flexing the neck slightly, and advance the tube until the mark reaches the nose (Figure 5)
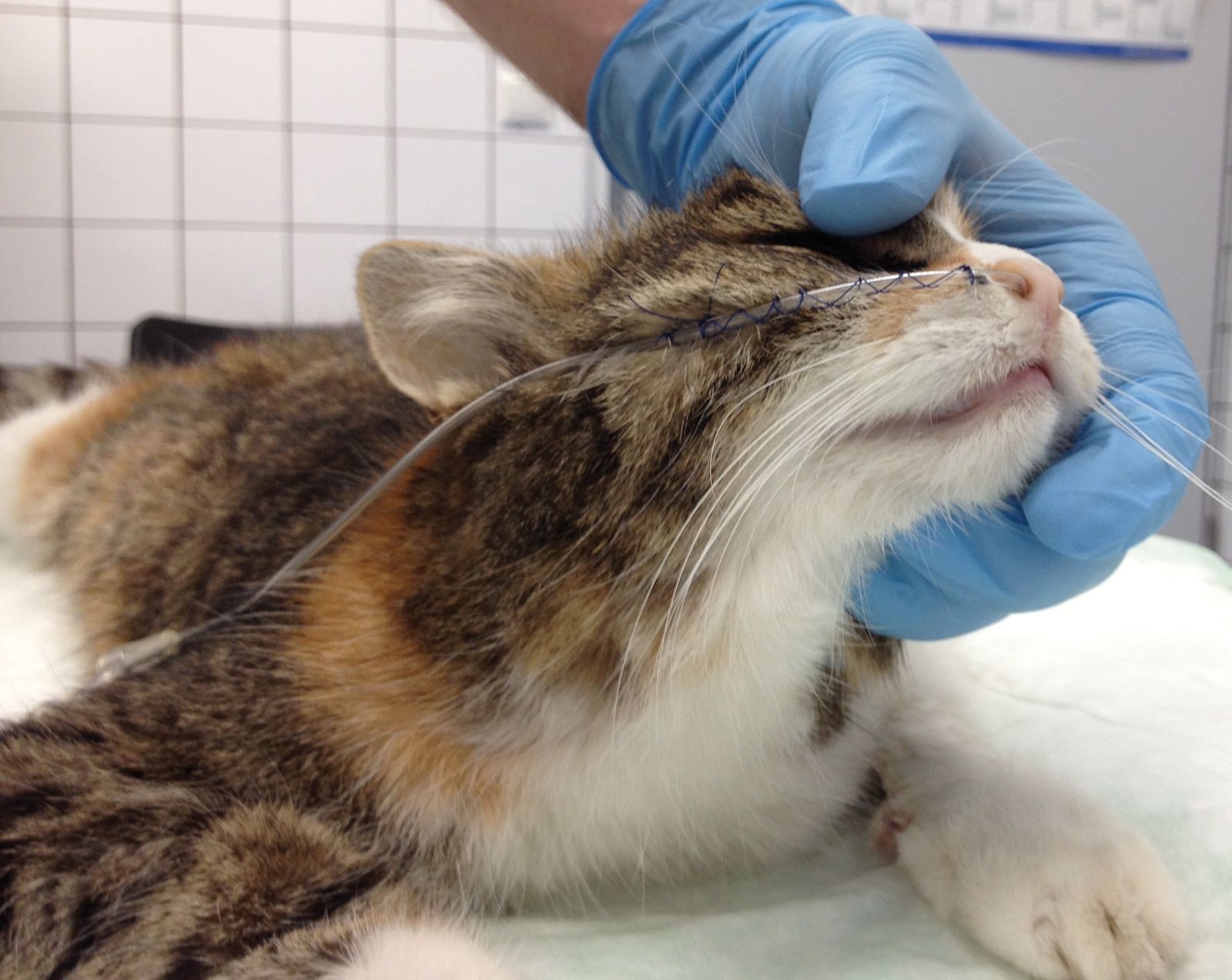
• Suture the tube using a Chinese finger trap; a second suture should be placed at the level of the upper jaw or on the forehead (Figure 6)
• As an alternative to suturing, tissue glue may be used, but note that, when the tube is removed, some hair (and possibly skin) may be removed as well
• Check positioning with radiography

Esophagostomy feeding tube
• Bypasses mouth and pharynx• Suitable for both liquid and slurry diets
• Can be left in place for many weeks if necessary
• Can be removed whenever required
• General anesthesia needed for placement
Materials required:
• Feeding tube 9-12 FG• Long Rochester-Péan forceps or equivalent (or a commercial esophageal tube introducer)
• Scalpel blade
• Skin disinfectant
• Suture material
• Needle holder
• Scissors
• Dressing materials
Placement technique:
• Anesthetize and intubate the cat• Place the cat in right lateral recumbency
• Clip and disinfect the left neck
• Measure tube length from mid-neck to the 8th intercostal space and mark with a permanent marker
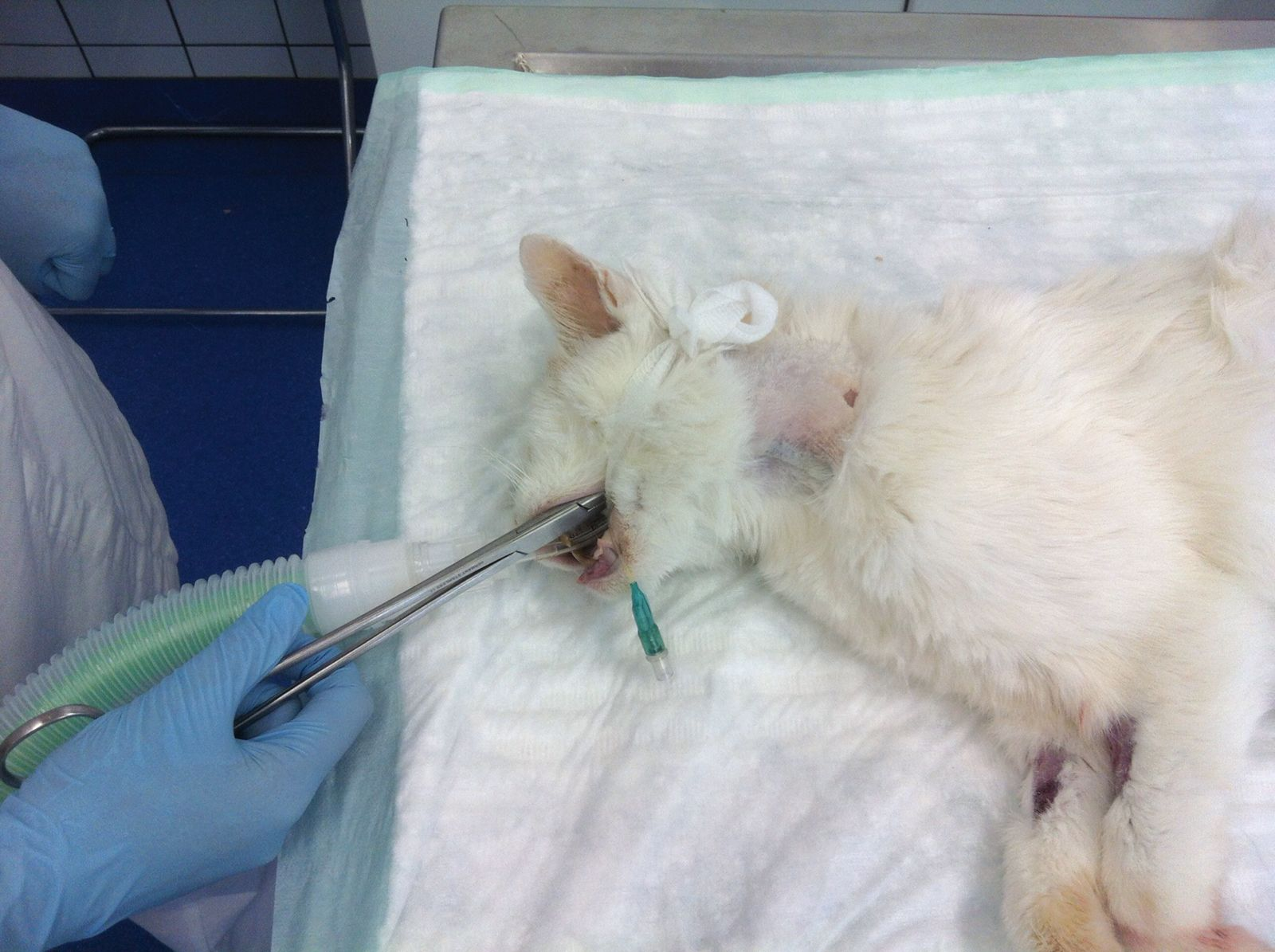
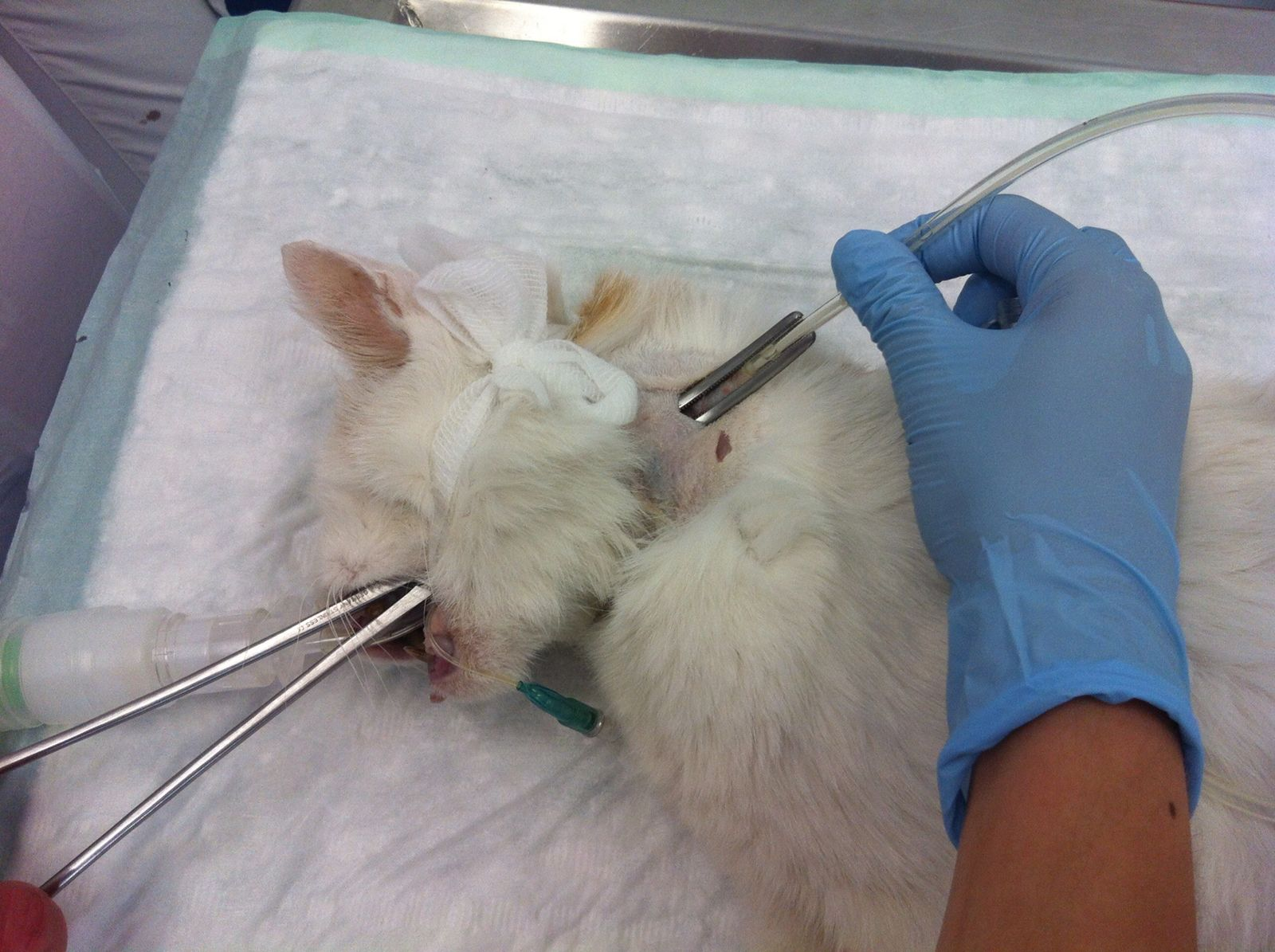
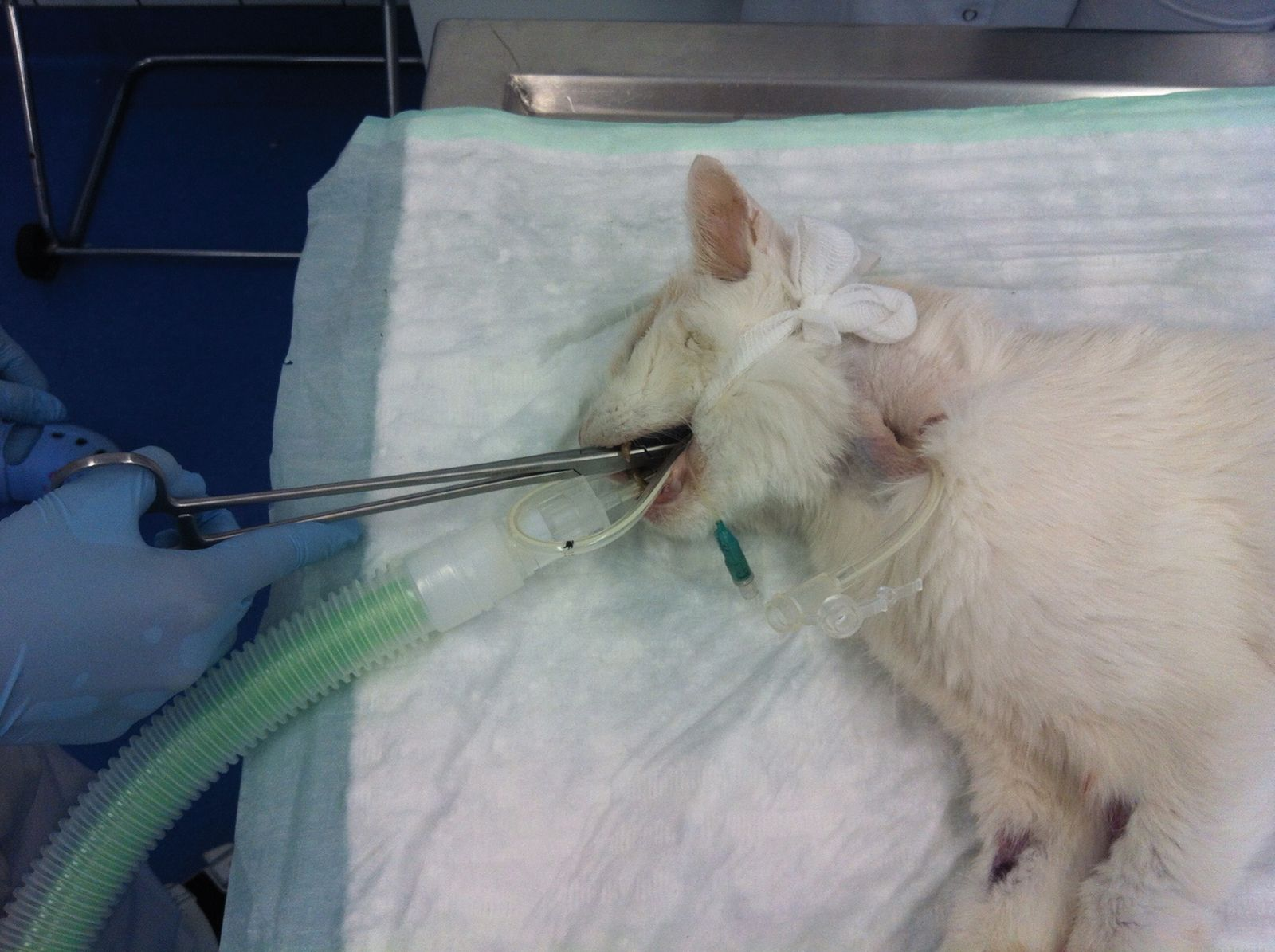
• Introduce the forceps into the esophagus from the mouth (Figure 7)
• Direct the tip of the forceps laterally until it can be felt dorsal to the jugular vein, then push the tip of the forceps towards the skin (Figure 8)
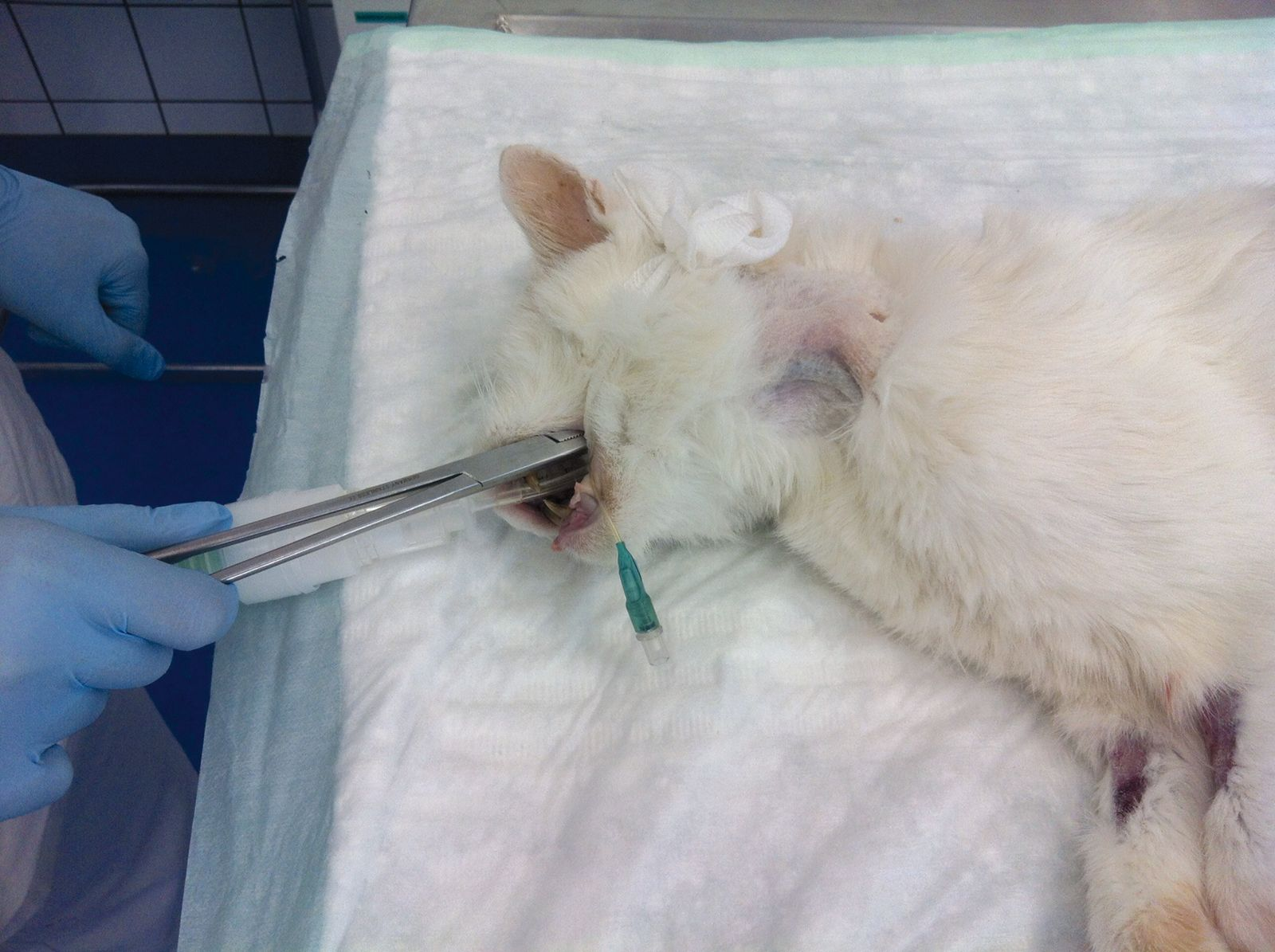
• Make a stab incision with the scalpel blade over the tip of the forceps (Figure 9) and push the forceps out through the skin incision (Figure 10)
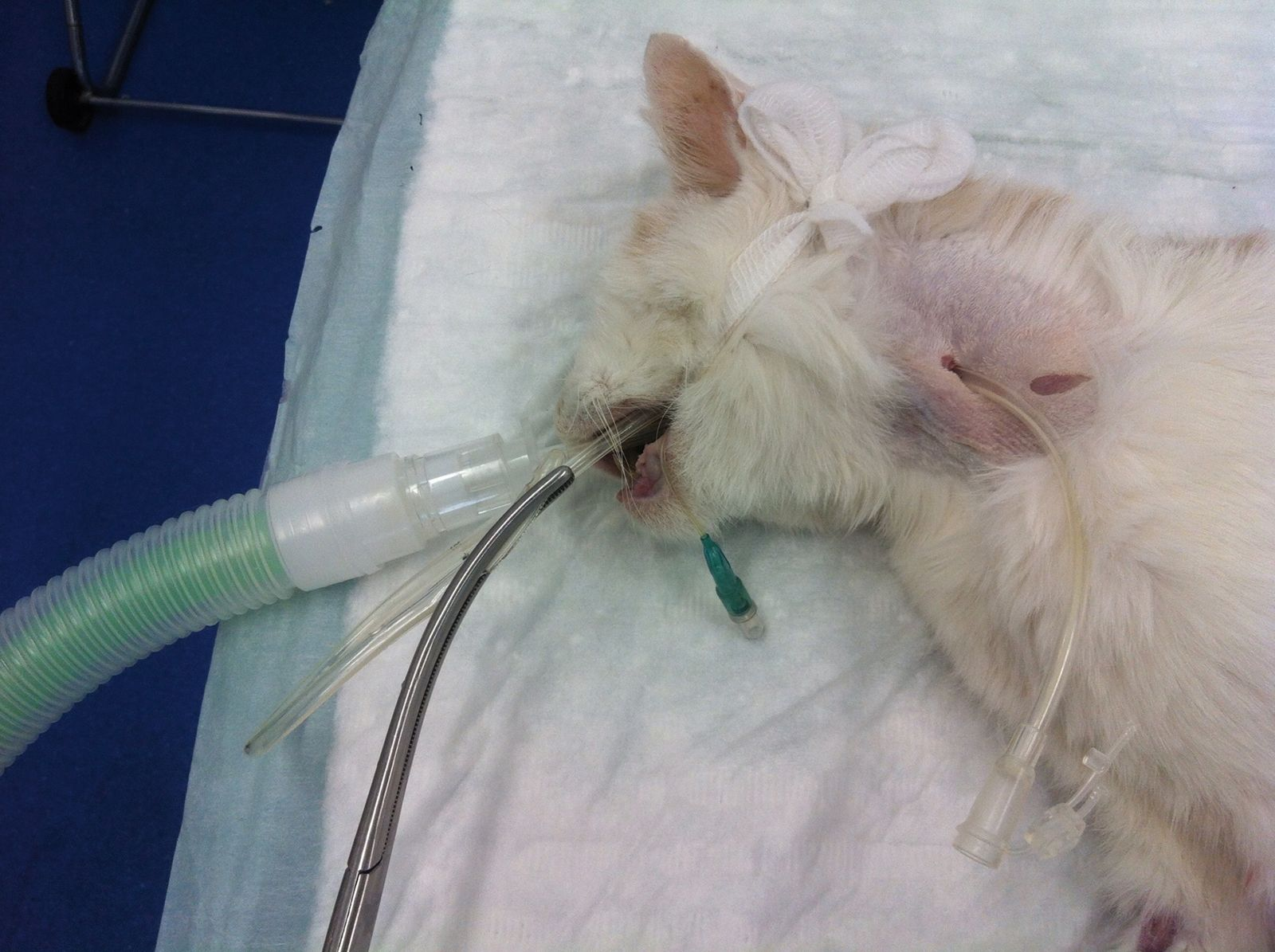
• Grasp the tube tip with the forceps (Figure 11) and withdraw the tube tip out of the mouth (Figure 12)
• Redirect the tube caudally into the esophagus (Figure 13)
• Advance the tube caudally until the tip of the tube is caudal to the skin incision, then maneuver the tube to ensure it is not kinked
• Advance the tube until the mark is level with the skin
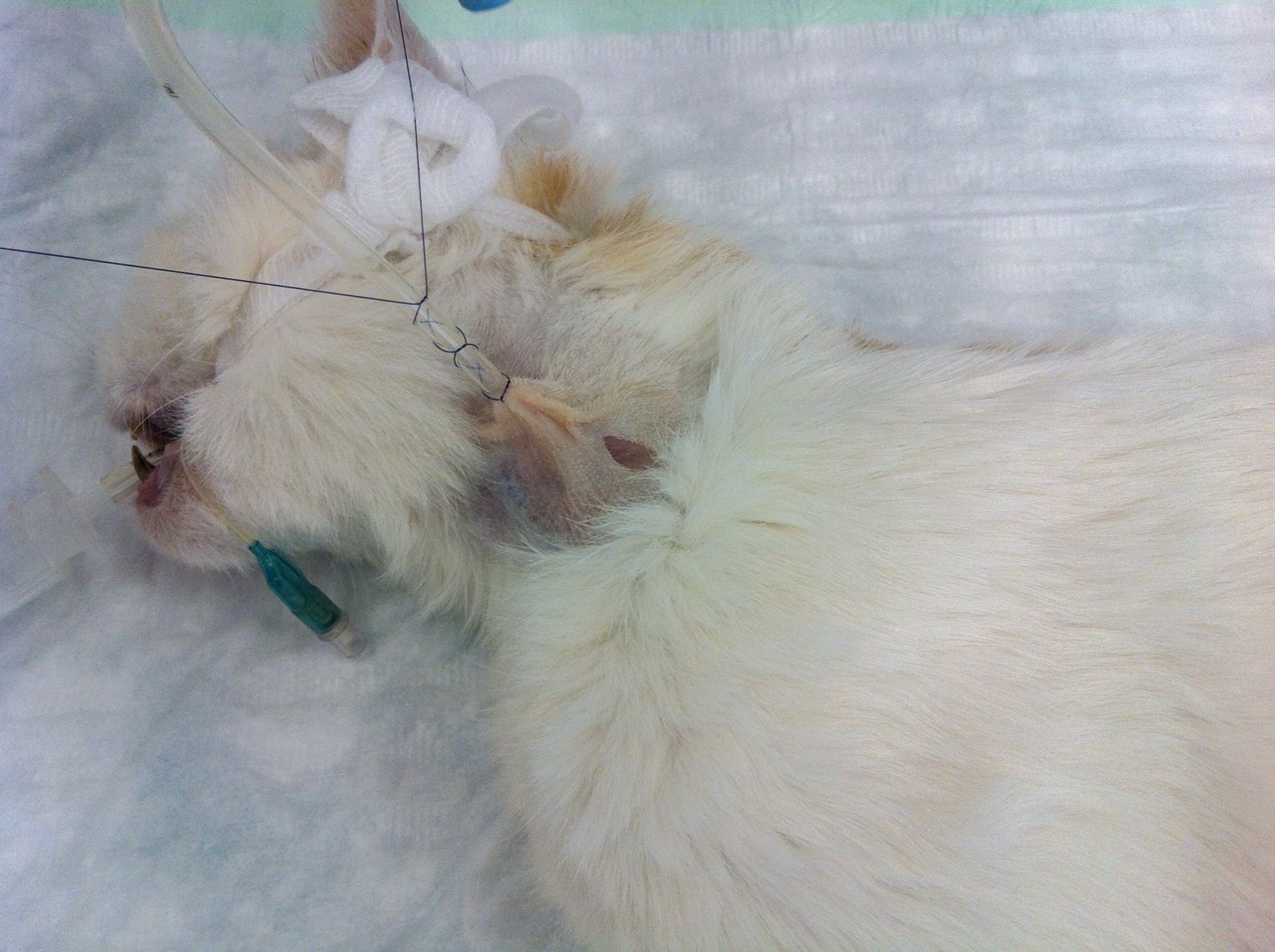
• Suture the tube in place using a Chinese finger trap (Figure 14)
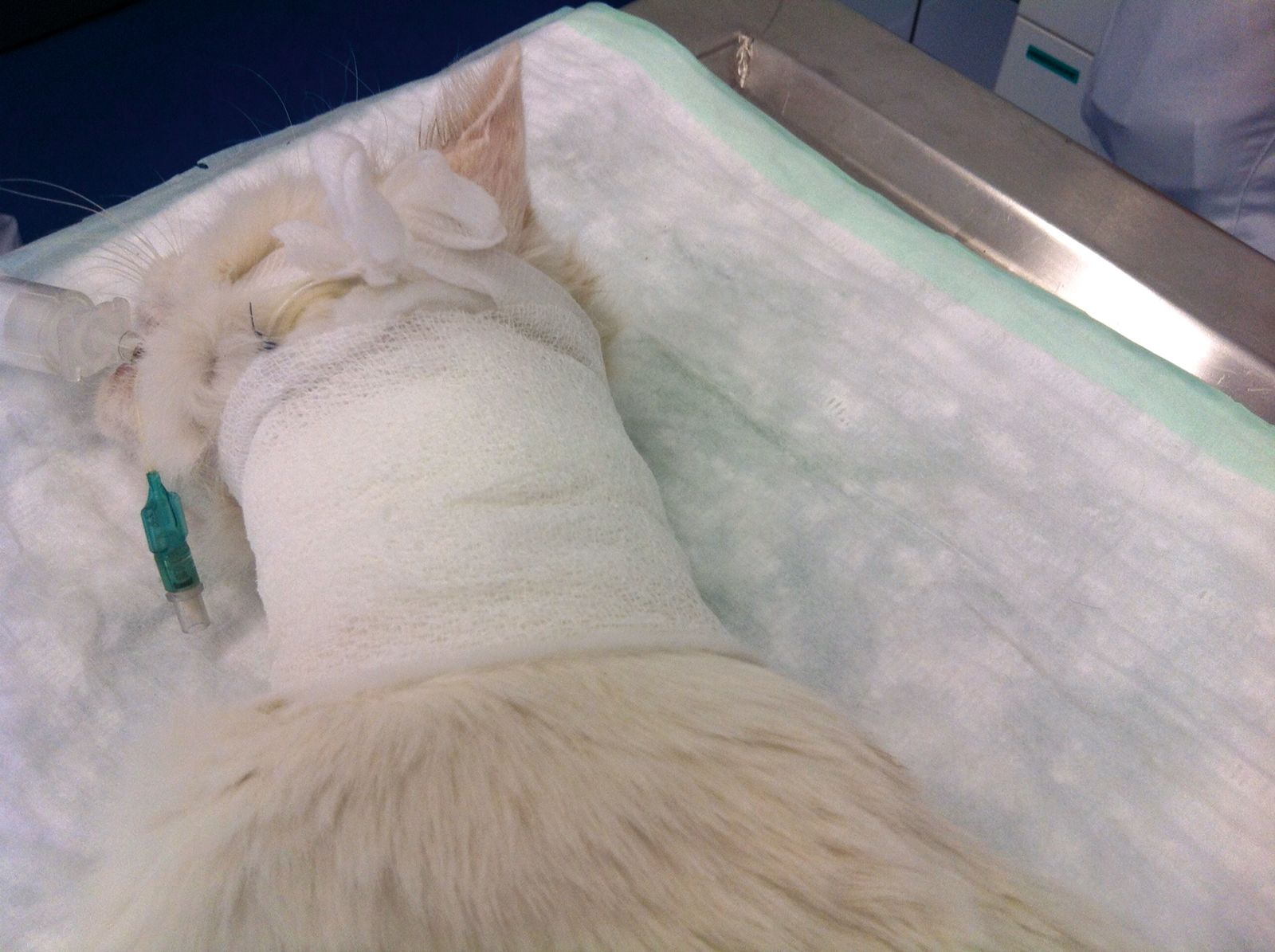
• Apply disinfectant lube around the insertion site and wrap the neck with bandages (Figure 15)
• Check positioning with radiography
Tube feeding technique
• Use food at room temperature
• Flush the tube before and after feeding with 2-3 mL of water
• Start with small boluses (1-2 mL/kg every 2-4 hours)
• Feed the cat 1/3 of its resting energy requirement* (RER) the first day, 2/3 RER the second and 3/3 RER the third day
• Increase bolus size stepwise up to 10 mL/kg (if tolerated by the cat)
• As an alternative to bolus feeding, a liquid diet can be given by constant rate infusion at a rate of 1-2 mL/kg/h. With this technique, the tube should be rinsed with water every 4-8 hours
*Daily RER can be calculated as follows: Kg0,75 x 70 = RER (kcal)
Rene Dorfelt
Dr. med. vet., Dip. ECVAA (Anesthesia and Analgesia)
Dr. Dörfelt studied at the University of Leipzig, Germany, qualifying in 2003. After completing a dissertation on hemodialysis and an internship at the Small Animal Clinic of the Freie Universität Berlin, he worked at the Norderstedt Veterinary Clinic in Germany from 2005-2007 before undertaking a residency in anesthesia and analgesia at Vienna’s University of Veterinary Medicine. Since 2011 he has been head of the Emergency and Critical Care Service at the Medical Small Animal Clinic of Ludwig Maximilian University in Germany.
Other articles in this issue
Share on social media